Table of Contents
I. Autoimmune Hemolytic Anemia
II. Antiphospholipid Antibody Syndrome (APS)
Autoimmune disorders occur when the immune system malfunctions and begins to attack the body’s organs and structures. Immune disorders can affect virtually every part of the body, including the circulatory system. This system is responsible for carrying blood to and from the heart. The circulatory system transports hormones, nutrients, and oxygen to cells while also removing waste products. [1]
Organs rely on blood for proper functioning, so if the blood starts to attack the body, several dangerous conditions can occur. Hemolytic anemia, vasculitis, and antiphospholipid antibody syndrome are three such diseases. Type 1 diabetes may also be classified as an autoimmune blood disease because of glucose buildup in the blood. Several anti-inflammatory medications may be prescribed to improve symptoms. Glucophage XR (metformin) is used for type 1 diabetes and prednisone for other vascular inflammation types. Read on to learn more about blood-related autoimmune disorders. [1]
Autoimmune Hemolytic Anemia
This condition refers to a group of autoimmune blood disorders. They are not especially common, but it is important to know the signs and symptoms. People with one autoimmune disorder are much more likely to develop another, so staying informed of possible accompanying issues like autoimmune hemolytic anemia is essential.
This disorder is characterized by the production of autoantibodies by the immune system. These autoantibodies attack red blood cells, treating them as foreign invaders to the body. Hemolytic anemia can occur at any age, and its cause is typically undetermined, but it often occurs alongside lymphoma, lupus, or viruses. If a virus causes it, then the red blood cells' destruction may stop over time. For others, this condition is chronic and can occur for long periods, if not a lifetime. The two types of hemolytic anemia include:
Warm antibody hemolytic anemia: This type occurs when autoantibodies attack and destroy red blood cells at normal body temperature
Cold antibody hemolytic anemia: This condition occurs when autoantibodies become active and attack red blood cells at temperatures below the normal body temperature. This condition is also known as cold agglutinin disease. [3]
Some people with hemolytic anemia may not experience any symptoms, so it is important to see your doctor regularly if you have lupus or lymphoma. This condition can be diagnosed with blood tests to determine the underlying cause of these autoimmune reactions. Some symptoms may include: APS occurs when the immune system attacks phospholipids. All living cells contain phospholipids, so if these substances are attacked, then serious conditions may occur. Antibodies typically help the body fight against invaders, but in the case of APS, they turn against the body and attack phospholipids. The attack and destruction of phospholipids can increase clotting in the blood vessels, resulting in an increased risk of stroke and heart attack. Around one to five percent of the population has APS. Women with this condition typically have a harder time getting pregnant or carrying a pregnancy to term. [2] Risk factors for APS include taking antibiotics for high blood pressure, blood infections (hepatitis C, HIV, or Lyme disease), family history of APS, and lupus. Blood tests are the most effective way of diagnosing APS as well as a physical exam. Symptoms of APS can vary significantly, depending on the seriousness of your case. If a blood clot is present, you may have a traditional stroke or heart attack symptoms. General symptoms can include: Pregnant women with APS may experience: Classic stroke symptoms can include: Vasculitis involves an inflammation of the blood vessels. The immune system attacks healthy blood vessels, causing the vessels to narrow and possibly burst. It affects around 200,000 people in the U.S. This disorder is typically classified by the size of the vessels affected. There is small-vessel vasculitis as well as medium and large vasculitis. Vasculitis can affect one organ or several and can occur for short periods or chronically. [2] The types of vasculitis can include: You may have an increased risk of developing vasculitis if you smoke, have chronic hepatitis B or C infections, or have another autoimmune disorder like lupus, scleroderma, or rheumatoid arthritis. Vasculitis symptoms vary and may be more severe if you experience this condition long-term. Other symptoms may be present if you experience vasculitis due to another disorder, like the ones listed above. If vasculitis is left untreated, you are at an increased risk of organ damage, blood clots, infections, or vision loss. General symptoms of vasculitis include: Like all autoimmune disorders, type 1 diabetes can affect almost every aspect of the body. Type 1 diabetes occurs when the immune system destroys insulin-making (beta) cells in the pancreas. In a normally functioning system, insulin hormones move sugar (glucose) into the body’s tissues for cells to use as fuel. When type 1 is present, glucose cannot fuel the cells and it builds up in the bloodstream. This leads to high blood sugar, leading to weight loss, damage to the eyes, kidneys, heart, dehydration, and diabetic ketoacidosis. Ketoacidosis occurs when the body breaks down fat cells when they cannot get enough glucose. This process creates ketones, which build up in the blood and can become life-threatening. Type 1 diabetes is typically diagnosed in early childhood or adolescence. Those with type 1 can live long and healthy lives; they just have to keep a close eye on their blood sugar levels and adjust their insulin depending on their diet. Type 1 diabetes cannot be prevented, and it is thought to be a genetic condition. [5] Before type 1 is diagnosed, several unpleasant symptoms may occur. Once type 1 is determined, people will be prescribed insulin treatments to control their blood sugar levels. Symptoms of type 1 may include: All blood-related autoimmune disorders have specific treatments. In type 1 diabetes, Glucophage XR (metformin) is used to increase insulin sensitivity. It stimulates glucose uptake, providing fuel for cells, and regulating blood sugar levels. This medication is used alongside insulin treatments, which can be administered via pump or injections. Anti-inflammatory drugs help reduce symptoms in vasculitis, APS, and autoimmune hemolytic anemia. Prednisone is a corticosteroid that reduces inflammation. Your doctor should monitor corticosteroid use because it can lead to severe side effects if you use corticosteroids for long periods. Other immune-suppressing medications like Imuran (azathioprine) can also be used alongside corticosteroids. [4] The content in this article is intended for informational purposes only. This website does not provide medical advice. In all circumstances, you should always seek the advice of your physician and/or other qualified health professionals(s) for drug, medical condition, or treatment advice. The content provided on this website is not a substitute for professional medical advice, diagnosis or treatment.
a. Symptoms
Antiphospholipid Antibody Syndrome (APS)
a. Symptoms

Vasculitis
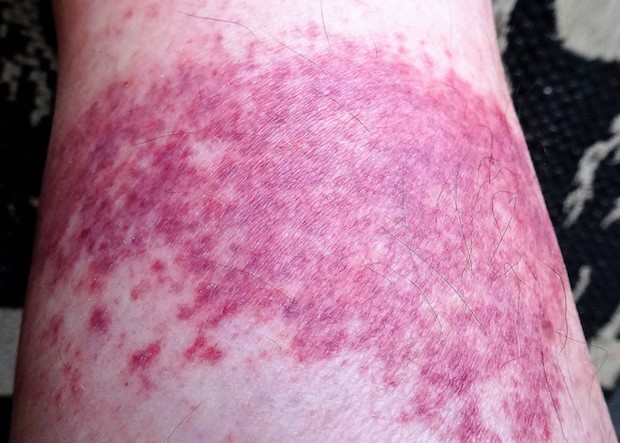
a. Symptoms
Type 1 Diabetes
a. Symptoms

Medications
