Table of Contents
I. Autoimmune Disorders and the Skin
Autoimmune Disorders and the Skin
Autoimmune disorders can affect every part of the body. If the immune system malfunctions, it can attack virtually any function within the body. The skin is the body’s largest organ, so it is often affected by immune system problems.
There are several types of skin-related autoimmune disorders. If you are experiencing an autoimmune skin disorder, your immune system mistakenly attacks the skin, leading to scleroderma, psoriasis, dermatomyositis, and epidermolysis bullosa. These disorders can severely impact your life if left untreated. Doctors may prescribe Rheumatrex (methotrexate) and Neoral (cyclosporine) to improve your symptoms. Read on to learn more about symptoms and treatment options for skin-related autoimmune disorders. [1]
Scleroderma
Scleroderma is a chronic connective tissue disease that affects over 300,000 people in the United States. Scleroderma is an autoimmune rheumatic disease, which refers to any disease that affects the cartilage, tendons, ligaments, skin, or muscles. Scleroderma comes from two Greek words: "sclero," meaning hard, and "derma," meaning skin. Scleroderma encapsulates a group of rare diseases that result in the hardening and tightening of the skin and connective tissues. Scleroderma occurs due to an overproduction of collagen and accumulation in the body's tissues. [2]
This disease is more common in women than men and typically occurs between 30 and 50. It is not contagious or infectious but occurs chronically. As scleroderma progresses, it can begin to affect blood vessels, internal organs, and the digestive tract. Your symptoms depend on the type of scleroderma you have. [3]
Your doctor will decide your treatment based on which part of the body scleroderma affects. Scleroderma can affect the following parts of the body: Skin: Almost everyone with scleroderma has skin hardening or tightening. This can occur in oval-shaped patches and may cover large parts of the torso and limbs. Your skin may look shiny because it is being stretched so tightly. These tight skin patches may impact your movements. Digestive system: If your stomach is affected by scleroderma, then several unpleasant symptoms can occur. This condition can weaken the intestines, and these muscles eventually become replaced with scar tissue. This muscle damage can cause cramps, diarrhea, constipation, or bloating. Absorbing nutrients from the intestines may become difficult, increasing your chance of malnutrition. Fingers and toes: Raynaud’s disease is one of the earliest signs of scleroderma. This disease involves a constriction of the small blood vessels in the fingers and toes. Your fingers and toes may begin to turn blue and feel numb. Heart, kidneys, and lungs: Heart and kidney disease is more common in those with scleroderma. If heart disease occurs, then they may experience chest discomfort and breathlessness. This occurs when the disease hardens heart muscles and veins, inhibiting blood flow. [3] Like many autoimmune disorders, this skin condition's exact cause is unknown, but doctors are fairly certain it is related to the immune system. Psoriasis causes red, itchy, and scaly patches to occur on the elbows, torso, knees, and scalp. Plaque psoriasis is the most common type, which results in raised patches of dry skin with silvery scales. Psoriasis is typically a genetic disease that does not have a cure. [4] The different types of psoriasis include: Psoriasis typically occurs in flare-ups, and medications like Rheumatrex (methotrexate) can help control symptoms. Flare-ups may occur due to infections, sunburns, medications, alcohol, and stress. You are more at risk for psoriasis if you have a compromised immune system and undergo chemotherapy or suffer from HIV. There are over 7.5 million people in the U.S. with psoriasis. Psoriasis can also result in psoriatic arthritis if left untreated. [1] Symptoms of psoriasis can vary greatly from person to person. The most common symptoms of psoriasis can include: Psoriasis can easily spiral out of control, and you may start shedding skin cells at a rapid rate. You should seek a doctor's help if these scales become widespread, cause discomfort, and impact your appearance. People with psoriasis may feel self-conscious and should seek treatment to help clear up unsightly skin patches. [4] This skin condition also causes skin redness, along with muscle weakness. Muscle weakness is more prevalent with dermatomyositis, but because it also affects the skin, it is often classified as a skin-related autoimmune disorder. It is also associated with polymyositis, another autoimmune disorder that causes soreness, stiffness, and muscle weakness. [1] This condition is most common in adults aged 40 to 60 and younger people between 5 and 15. Dermatomyositis is typically degenerative, leading to muscle wasting and stiff joints. Doctors have to do a skin and muscle biopsy to determine dermatomyositis. This piece of tissue will be examined underneath a microscope for proper diagnosis. [5] Dermatomyositis symptoms may appear suddenly, and the skin rash often occurs before muscle weakness. The lungs, as well as the digestive tract, may also be affected as time goes on. Symptoms of dermatomyositis can include: Epidermolysis bullosa is a group of diseases that cause blistering and fragile skin. Epidermolysis Bullosa is typically inherited, and blisters may occur due to minor injuries, heat, scratching adhesive tape, or friction. Most people recognize the presence of this disease as toddlers or small children. The blisters may appear when a small child starts physical activities like walking or running, and the skin experiences friction. This disease has no cure, but the mild forms often improve with age. The three main types of this condition include: Epidermolysis bullosa simplex: This most common form develops on the outer layer of skin and affects the palms and feet. These blisters usually heal well and do not scar. Junctional epidermolysis bullosa: This type is severe and typically begins in infancy. Babies may develop a hoarse-sounding cry from the blistering and scarring of their vocal cords. Dystrophic epidermolysis bullosa: This is due to a genetic defect that produces collagen that strengthens the skin. If this gene is missing, then the skin layers do not join properly and can cause rashes. There are many symptoms of epidermolysis bullosa, and the severity varies greatly. This condition is often diagnosed through genetic testing or skin biopsy. Common symptoms can include: Over time, many complications of epidermolysis bullosa can occur. It can lead to dental problems, constipation, the fusion of fingers and joint changes, skin cancer, and infection. Infection is a major concern with open blisters, so keeping the blisters as clean as possible is essential. [6] All of these autoimmune skin disorders have specific treatments. The repeated scarring of the skin and internal organs can lead to impaired mobility and malnutrition. So, in epidermolysis bullosa and scleroderma, people often have to pair rehabilitation therapies with medications to maintain normal functioning. [6] Overall, several similar medications can help suppress the immune system and improve skin-related immune system problems. Rheumatrex (methotrexate) is used to treat severe psoriasis by reducing the function of cells that cause inflammation. Neoral (cyclosporine) can also be used for skin-related autoimmune disorders because of its immunosuppressant abilities. Neoral prevents the body from attacking its organs and structures, reducing inflammation. These drugs should be used with caution, especially methotrexate. Talk to your doctor about a treatment plan for your skin-related autoimmune disease. [7] The content in this article is intended for informational purposes only. This website does not provide medical advice. In all circumstances, you should always seek the advice of your physician and/or other qualified health professionals(s) for drug, medical condition, or treatment advice. The content provided on this website is not a substitute for professional medical advice, diagnosis or treatment.
a. Symptoms
Psoriasis
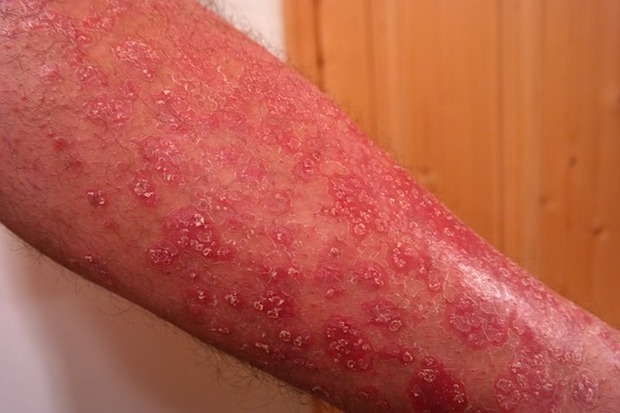
a. Symptoms
Dermatomyositis
a. Symptoms

Epidermolysis Bullosa
a. Symptoms

Treatments
